In recovery, people often refer to avoiding addiction triggers. What are triggers, and why do they matter?
An addiction trigger can be anything that prompts memories, thoughts, or feelings that have to do with addiction.
How do addiction triggers work?
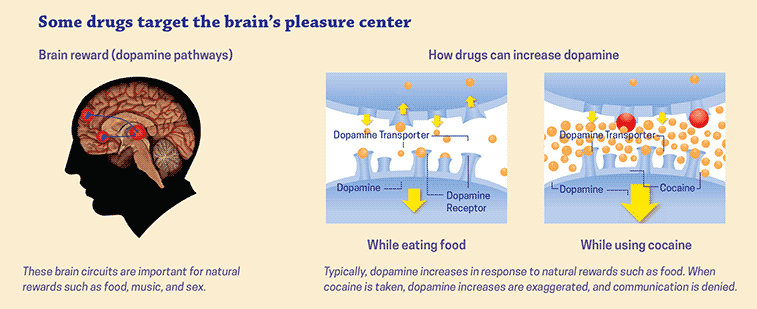
In order to fully understand addiction triggers, we must first understand how addiction rewires the reward circuitry in the brain. Our brains are programmed for survival. This means we naturally avoid pain (like fire) and seek out pleasure (like eating sweet, nutritious fruit). We feel good after we exercise or chat with a friend because these healthy behaviors affect us in a positive way, and we get a mild boost of feel-good chemicals in our brains from them. Addiction hijacks this natural reward circuitry, as drugs flood our brains with feel-good chemicals. Eventually, those of us with addiction become acclimated to these larger doses of chemical rewards, and will go to dramatic lengths to achieve a buzz.
The illustration above, from NIDA shows how drugs can affect the feel-good chemicals in the brain.
As we begin to anticipate the big boosts of feel-good chemicals coming from our next fix, even the events and activities associated with the addictive behavior can cause changes in our brain. This is where triggers (or ‘cues,’ as they’re sometimes called in the science world) come in. Anything associated with the memories, thoughts, or feelings of addiction can be a trigger. It can cause your brain to reboot to the broken reward circuitry, resulting in cravings for drugs, alcohol, or behaviors even long after you’ve given them up.
Another thing to remember? In early recovery, the lack of extra feel-good chemicals coming from our substance or behavior of choice causes us to feel out-of-wack. Our brain stops making as many natural feel-good chemicals, because it’s accustomed to getting a boost from the substances we’ve been using. Samantha Panek, LLMSW, explains, “We’re especially desperate for feel-good chemicals in early recovery because they have become depleted. It’s like a flood of unbalanced emotions, feelings, and anxiety when people stop using.”
Why do addiction triggers matter?
Addiction can feel hopeless, but the more each of us understand about how addiction works, the better equipped we are to be active participants in our own recoveries. It can often feel like a relapse comes out of the blue, when in fact triggers led us towards it.
Identifying our own triggers, and learning to navigate through addiction triggers as a part of the recovery process, can help us avoid relapse and handle sticky situations. When we find ourselves craving our substance or behavior of choice, we can try to track back to recent events: how am I feeling? Did anything specific happen recently? We may find new insight about situations, people, or feelings that lead us back towards our addiction. Remember that even when we experience triggers, we still have the ability to make choices about how we respond to them. Encountering a trigger doesn’t force us to drink or use.
“We’re especially desperate for feel good chemicals in early recovery but especially low on them naturally. It’s like a flood of unbalanced emotions, feelings, and anxiety when people stop using.”
What are common addiction triggers?
Emotions: Both positive and negative emotions can be triggers for people in recovery. Why? For many of us, we masked our real emotions with our addiction of choice, and used substances or behaviors to cover them up whenever they would arise. This makes emotions, a natural aspect of human life, a trigger.
People, Places, & Things: If you drank in a specific bar every night, walking back into that bar in recovery will set your brain up to anticipate a drink. The same is true for the people that we used drugs, drank, or practiced behaviors with, and things like drug paraphernalia or even an old journal. This is why in early recovery, it is often encouraged to evaluate relationships and ensure you can avoid risky situations and environments.
I asked some friends in recovery about their own addiction triggers and how they cope with them. Robin, Workit Health’s Co-Founder, explained that “walking through the liquor aisle at the grocery store, family stress at the holidays, and sitting on the plane when the person next to me is drinking wine” are all triggers for her. She handles each of them differently: “I order groceries on Amazon Prime, if I’m on a flight I’ll ask to change seats or put on lots of scented moisturizer so I can’t smell the wine, and I reach out to my AA community for support during the holidays.”
My friend Lisa has trigger-mapping down to a science. Her triggers? “The afternoon energy slump, grief about the existence of death, conflict avoidance, holidays, evening chill time alone, jealousy and fear, being out of shape i.e. lethargic, awkward social networking events like happy hours that put me in a big group.” She keeps track of each of her triggers, along with the apps and tools she can use to combat them.
Our friend Corissa noted that along with drug paraphernalia, certain bands and musicians are triggering for her. She avoids listening to them in recovery, but says, “When they come on the radio or if someone else plays them, I can’t help but think of old times.“
So how can you cope with addiction triggers?
Addiction triggers sound scary. But understanding your triggers and finding healthy coping skills to manage your own emotions, instead of going back to your addiction, can be empowering.
For people and places, avoidance is a common solution. If you know certain people or places are triggering for you, then try to avoid those people or places. For other triggers, like emotions, avoidance isn’t an option. This is where healthy coping skills are crucial.
Common coping skills that can help you navigate triggers in recovery:
-
Talking with your support system, like a recovery coach or therapist, your sponsor, or supportive family members or friends.
-
Mindfulness, like taking five deep breaths, taking a walk around the block to unplug, or doing a five-minute meditation from your favorite meditation app.
-
Checking your HALT. HALT is an acronym that stands for Hungry, Angry, Lonely, and Tired, all feelings that can not only be triggering themselves, but can also make our defenses lower when facing other triggering emotions or events.
If this all sounds overwhelming, fear not. ust becoming aware of triggers and the way addiction has affected the reward circuitry of our brain is the first step towards positive change. Just reading about triggers, and gaining knowledge about how you can act differently when presented with them in the future, can set you up on the path for success.