Reaching Rural Communities
Members can access science-backed treatment for substance use disorder, even when they live in rural areas and treatment deserts far from providers.

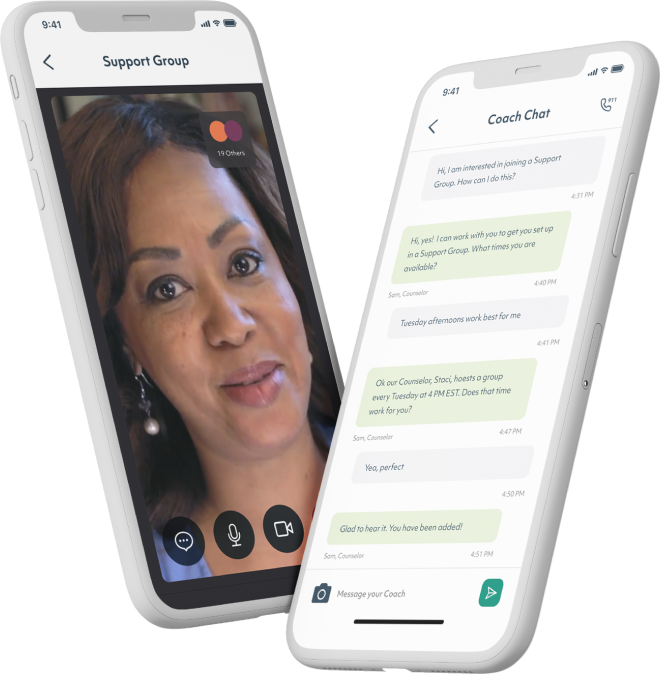
Workit Health's model provides access for rural members
The burden of drug use and overdose is high in rural communities where accessing treatments can be difficult. 28 million Americans live more than 10 miles from the nearest buprenorphine provider. Workit Health brings a full clinical program for opioid use disorder right to members’ hands via our custom app, so that rural members can get the care they need. Almost a quarter of Workit Health members live in rural areas. Members receive:
- Clinical and behavioral health support
- Community connection for peer support
- At-home urine drug screens
- Medications e-prescribed to a local pharmacy (when clinically appropriate)
- Treatment for co-occurring conditions
- Technology that is simple to use and streamlined across devices
- Responsive care team via in-app chat messaging
Expert clinical care without the travel
Through the Workit Health app, members attend video visits with a medical provider, access recovery groups, and complete an interactive curriculum of skills-based courses. Members have a frictionless experience, attending video visits with dedicated clinicians who are licensed in their state and picking up their prescriptions, including buprenorphine, at their local pharmacies. People who once had to travel hours every day to receive medication can now receive opioid use disorder care from the comfort of their own homes.

Demonstrated success in reaching rural populations
In 2017, Workit Health opened our first clinic in Michigan, where a large portion of the state is rural. In Michigan’s Upper Peninsula, the northernmost landmass of the state, the average distance to a buprenorphine clinic is 63.3 miles, and Michigan counties lacking an emergency department are all located within the Upper Peninsula.
Since 2019, the number of Workit Health members in the Upper Peninsula of Michigan who have attended a clinical appointment for opioid use disorder has risen 300%. And in rural zip codes across the Lower Peninsula of Michigan, there has also been significant growth, with an increase of more than 200%. These rural members report that the change is life-altering, saving them hours of travel each month. Workit Health’s impact on rural areas is not confined to Michigan. Similar growth has taken place in rural areas of other states as we’ve expanded. Currently, nearly a quarter of Workit Health members live in rural areas. Click here to learn more about Workit Health’s impact in rural areas from our Chief Medical Officer Justin Coffey, M.D.
Need more information? We can reach out to you.
Fill out this form for more information or to schedule a call. Or feel free to reach out by email or phone:
Citations
1. Buprenorphine. Substance Abuse and Mental Health Services Administration (SAMHSA). https://www.samhsa.gov/medication-assisted-treatment/medications-counseling-related-conditions/buprenorphine. Accessed November 2021.
2. Davis, C. S., & Samuels, E. A. (2021). Continuing increased access to buprenorphine in the United States via telemedicine after COVID-19. The International Journal on Drug Policy, 93: 102905. https://doi.org/10.1016/j.drugpo.2020.102905
3. Langabeer, J. R., Stotts, A. R., Cortez, A., Tortolero, G., & Champagne-Langabeer, T. (2020).
Geographic proximity to buprenorphine treatment providers in the U.S. Drug and Alcohol Dependence, 213. https://doi.org/10.1016/j.drugalcdep.2020.108131
4. Mahmoud, H., Naal, H., Whaibeh, E., & Smith, A. (2022). Telehealth‑Based Delivery of Medication‑Assisted Treatment for Opioid Use Disorder: a Critical Review of Recent Developments. Current Psychiatry Reports, 24:375–386. https://doi.org/10.1007/s11920-022-01346-z
5. Hughes, P. M., Verrastro, G., Fusco, C. W., Wilson, C. G., & Ostrach, B. (2021). An examination of telehealth policy impacts on initial rural opioid use disorder treatment patterns during the COVID-19 pandemic. The Journal of rural health : official journal of the American Rural Health Association and the National Rural Health Care Association, 37(3), 467–472. https://doi.org/10.1111/jrh.12570
6. Dora-Laskey, A., King, A., & Sadler, R. (2022). Identifying barriers to emergency department-initiated buprenorphine: A spatial analysis of treatment facility access in Michigan. The American Journal of Emergency Medicine, 51, 393-396. https://doi.org/10.1016/j.ajem.2021.11.014